- What is a vasectomy?
- History of the vasectomy
- Who uses vasectomy?
- Effectiveness of vasectomy
- Who should and should not have a vasectomy?
- Before surgery
- The surgery
What is a vasectomy?
Vasectomy is a surgical procedure for male sterilisation, that is, surgery which makes a man unable to conceive. It involves severing the vas deferens (the tube linking the testicles to the ejaculatory ducts in the penis) and in most cases blocking or tying one or both of the severed ends. This effectively blocks the path by which sperm leave the testes and therefore makes a man permanently sterile.
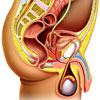 |
For more information on the anatomy of the reproductive system, see Male Urogenital System. |
History of the vasectomy
In Australia, sterilisation of either males or females was considered illegal and immoral until the 1970s. Through the agitation of Dr Ian Edwards, a Sydney doctor in the 1970s, Humanist Societies in each Australian state gave ethical clearance to the procedure, as did the Australian Medical Association. Through practice, the procedure came to be regarded as legal in all Australian states except Queensland. Vasectomy rapidly gained popularity; some 27,000 procedures were performed in 1974.
Who uses vasectomy?
Vasectomy is a permanent method of male sterilisation and is therefore used by men who have no wish to father children in the future, and who wish to eliminate the risk of their partner/s conceiving. Sterilisation (of both men and women) is now the principle method of contraception used throughout the world. Globally, some 42 million men have previously undergone vasectomy. In the United Kingdom, 64,422 vasectomies were performed in 1999, and 15% of all British men aged 16–64 had undergone the procedure in 2001.
In Australia, more than 30,000 vasectomy procedures are performed each year and it is estimated that one in four men will have a vasectomy at some point in his life.
Effectiveness of vasectomy
Vasectomy is a highly effective method of permanent contraception. In the early stages following a vasectomy (i.e. the first six months) there is a failure rate of around 2%, mainly due to spontaneous recanalisation (the growth of small tubes linking the severed ends of the vas deferens, creating an alternative route via which sperm can travel from the testes to the ejaculatory ducts). However, failure of the procedure at this stage is generally picked up during post-vasectomy semen analysis, before the man is given clearance to stop using alternative contraceptives. Early failure should not therefore result in unwanted pregnancy, and failed procedures can be repeated.
Unwanted pregnancy occurs after approximately 1 in 2,000 vasectomy procedures, although the actual failure rate after initial clearance to cease contraceptive use is given appears to be much higher. One study, involving 30,000 vasectomised men who underwent semen analysis testing each year following successful vasectomy, reported a failure rate of 1 in 165 men (0.65%) after three years.
Who should and should not have a vasectomy?
Vasectomy is indicated when individuals, who are of sound mind and not acting under external duress, request the procedure. As vasectomy is a permanent method of contraception, it is appropriate only for men who do not wish to have children in the future. Doctors and other health professionals are likely to emphasise the permanent nature of the procedure to individuals requesting a vasectomy.
In some cases where the man seeking treatment has an infection or abnormality of the genitals, vasectomy may not be possible, or consultation with a specialist (e.g. a urologist) may be necessary.
Vasectomy should be delayed if men have infections around the scrotum, or in the vas deferens or epididymis, until the infection has been treated. These infections, which are often sexually transmitted, increase the risk of postoperative infections.
The presence of a lump in the scrotum may indicate an underlying condition (e.g. testicular cancer), and men with a lump in the scrotum may be referred to a specialist.
Similarly, men may be referred to a specialist if they have a history of:
- Cryptorchidism;
- Inguinal hernia;
- Coagulation disorders;
- Scrotal trauma; or
- Large varicocoele or hydrocoele.
Before surgery
Clinical examination and history taking

Infections should be treated before starting surgery. In cases of genital abnormalities that may interfere with the procedure, specialist referral may be necessary.
Counselling is routinely performed before vasectomy. In most cases, the counsellor will discuss the procedure with both the man and his partner. Some men wishing to undergo vasectomy are single, or do not wish their partner to know about the procedure, and are counselled alone. The procedure is permanent, so it is important that the men or couples seeking a vasectomy are well informed about the potential risks and benefits of the procedure.
Pre-vasectomy counselling will usually involve a thorough discussion of the procedure, as well as alternative contraceptive options available to the man or couple. It will provide an opportunity for them to ask any questions and raise any concerns they have regarding the procedure. The risks, benefits, advantages and disadvantages of vasectomy should be outlined by the counsellor, who is likely to emphasise that the procedure is permanent and irreversible in most cases, though it has a failure rate of around 2% in the early stages.
Information regarding the possibility of surgical sperm retrieval and conception through the use of assisted reproductive techniques (e.g. intracytoplasmic sperm extraction) may also be offered.
Generally the man or couple will be provided with booklets or other printed materials outlining the information covered in the counselling session.
Men should also be informed of the need to use contraceptives after the procedure is done until sterilisation has been confirmed through semen analysis. After the counselling session, the man undergoing vasectomy will usually be asked to sign a consent form stating that he agrees to undergo the procedure and confirming that he has received comprehensive counselling about the intended vasectomy.
The surgery
Vasectomy is a simple surgical procedure that takes around 15 minutes and can be performed in a clinic or hospital under local or general anaesthetic. In most cases, and whenever possible, the procedure should be conducted under local anaesthetic, due to the additional risks and recovery time associated with general anaesthetic.
The vasectomy procedure involves two distinct stages. First the vas are accessed and severed. Secondly the severed ends of the tube are tied or blocked. These modifications prevent sperm travelling from the testes to the ejaculatory ducts.
There are two techniques that can be used in the first stage of vasectomy surgery (i.e. severing the vas deferens), known as the scalpel and no scalpel techniques.
In the scalpel technique, the surgeon will make small incisions in the scrotum, through which each vas deferens is pulled. The vas is then cut. A 1–3 cm section may be removed.
The no scalpel technique uses a specially designed clamp and a small, pointed forceps-like device to hold and puncture the vas deferens. Evidence suggests that the no scalpel approach results in fewer early complications (e.g. infection, haemorrhage), reduces operating time, and enables a faster return to sexual activity for the patient. However, the no scalpel technique requires greater experience on the part of the surgeon and may not always be practical.
- Ligation: Ligation involves tying off the ends of the vas deferens with silk or cotton. It is the most commonly applied technique in resource-poor settings, but is less popular in developed countries because of its higher failure rate (around 18% of vasectomy procedures in the United States involve ligation, compared to around 95% in India, Bangladesh and Nepal).
- Clipping: Clipping is a procedure in which clips are applied to the ends of the vas deferens. The procedure is not recommended where other methods are available, due to the increased risk of failure.
- Cautery or diathermy: In the cautery or diathermy procedure, heat is applied to the tube ends of the vas. Cautery is the most common technique used for vasectomy in the United States (71% of vasectomies undertaken in 1995 used the technique), and has an overall failure rate of < 1%. However, reversal of a vasectomy involving cauterisation is less likely to succeed.
- Fascial interposition: Fascial interposition is a procedure in which the spermatic tissues surrounding the vas are pulled over one end of the severed vas to create a natural barrier.
Evidence demonstrates that, for optimal results, division of the vas deferens should be combined with fascial interposition and/or diathermy. Division of the vas deferens alone or with clipping or ligation techniques should be avoided due to the high failure rates associated with these procedures.
After surgery
Semen analysis is conducted after the vasectomy to assess whether or not sperm stored in the epididymis and ejaculatory gland has been cleared, and whether or not the procedure was successful. In other words, semen analysis testing is conducted to make sure there is no sperm in the semen of a vasectomised man. It is a crucial step in the vasectomy process as, until it is confirmed, the man remains potentially fertile and must continue to use alternative contraceptive methods.
The timing and number of semen analysis tests conducted vary between practitioners and nations. The timing of semen analysis testing can be calculated in terms of a period of time which has elapsed following the operation (e.g. three months), the number of times a man has ejaculated after the operation, or a combination of the two.
In Australia, the Royal Australia College of Surgeons recommend a post-vasectomy semen analysis test three months and at least 20 ejaculations after the procedure to confirm sterility. No repeat testing is recommended for men whose semen sample is free of sperm at this time. If sperm is present in semen in the initial test, periodic testing is recommended until no more sperm is found.
British guidelines recommend repeat semen analysis testing of all vasectomised men 12 and 16 weeks after the procedure, regardless of the initial test result.
In instances where the lack of sperm is not confirmed but only immotile sperm are found in the sample at a concentration of < 10 million/mL of ejaculate, special clearance can be given to cease contraceptive use. While the risk of pregnancy is still theoretically possible with such low sperm concentrations, post-vasectomy pregnancy has not been recorded in men with a sperm count of < 10 million/mL.
Vasectomy reversal

Vasectomy is successfully reversed in some 50% of men seeking reversal. The success rates are influenced by the method of vasectomy used and the time elapsed since the procedure was performed. Vasectomies using diathermy or cauterisation techniques, and those in which sections of the vas were excised, are less likely to be successfully reversed. Men who are younger at the time of vasectomy and who seek reversal after a relatively short period of time are more likely to experience successful reversal.
Risks of a vasectomy
There are no known long term health risks associated with vasectomy. No association has been found between vasectomy and testicular cancer or heart disease, and there is no evidence that the increased risk of prostate cancer associated with vasectomy is causative.
Men may experience chronic testicular pain after the procedure. Up to 5% of men seek medical attention or report reduced quality of life as a result of this complication. In the short term, there is also an increased risk of kidney or bladder infections, and of orchitis and epididymitis.
For most men, the procedure is irreversible. Therefore there is a risk of being unable to conceive in the future should it be desired. Around 3% of Australian men who have a vasectomy attempt conception in the future, either by reversal of the vasectomy or through assisted reproductive techniques.
Benefits of a vasectomy
Vasectomy is an effective and safe means of permanent sterilisation that does not interfere with the normal sexual functioning of a man. After a vasectomy, men still produce sperm, achieve orgasm and ejaculate (although the ejaculate will no longer contain sperm).
More information
 |
For more information on different types of contraception, male anatomy and related health issues, see Contraception. |
References
- Royal College of Obstetricians and Gynecologists. Male and Female Sterilisation: Evidence Based Guideline Number 4 [online]. London: RCOG Press; 2004 [cited 15 February 2009]. Available from URL: http://www.rcog.org.uk/ files/ rcog-corp/ uploaded-files/ NEBSterilisationFull060607.pdf
- Cook LA, Van Vliet H, Lopez LM, et al. Vasectomy occlusion techniques for male sterilization. Cochrane Database Syst Rev. 2007;(2):CD003991. [Abstract | Full text]
- Leavesley JH. Sterilisation through vasectomy in Australia. Presented at the Reproductive Health Care International Symposium. Maui, Hawaii; 1982: 7.
- Vasectomy [online]. Andrology Australia. 1 December 2005 [cited 19 February 2009]. Available from URL: http://www.andrologyaustralia.org/ pageContent.asp? pageCode=VASECTOMY
- Haldar N, Cranston D, Turner E, et al. How reliable is a vasectomy? Long-term follow-up of vasectomised men. Lancet. 2000;356(9223):43-4. [Abstract]
- Gingell C, Crosby D, Carroll R. Review of the complications and medicolegal implications of vasectomy. Postgrad Med J. 2001;77(912):656-9. [Abstract | Full text]
- Li SQ, Goldstein M, Zhu J, Huber D. The no-scalpel vasectomy. J Urol. 1991;145(2):341-4. [Abstract]
- Cook LA, Pun A, van Vliet H, et al. Scalpel versus no-scalpel incision for vasectomy. Cochrane Database Syst Rev. 2007;(2):CD004112. [Abstract | Full text]
- Aradhya K, Best K, Sokal DC. Recent developments in vasectomy. BMJ. 2005; 330(7486): 296-9. [Full text]
- Sokal D, Irsula B, Hays M, et al. Vasectomy by ligation and excision, with or without fascial interposition: A randomized controlled trial. BMC Med. 2004;2:6. [Abstract | Full text]
- Hancock P, McLaughlin E. British Andrology Society guidelines for the assessment of post vasectomy semen samples. J Clin Pathol. 2002;55(11):812-6. [Abstract | Full text]
- Griffin T. Post-vasectomy testing to confirm sterility [online]. Royal Australasian College of Surgeons. 21 January 2004 [cited 19 February 2009]. Available from URL: http://www.surgeons.org/ Content/ ContentFolders/ News/ ASERNIPS/ Systematicreviews/ PVTexecsum1203.pdf
- Holman CD, Wisniewski ZS, Semmens JB, et al. Population-based outcomes after 28,246 in-hospital vasectomies and 1,902 vasovasostomies in Western Australia. Br J Int. 2000;86(9):1043-9. [Abstract | Full text]
- McDonald SW. Is vasectomy harmful to health? Br J Gen Pract. 1997;47(419):381-6. [Abstract | Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







